Conditions managed related to Ear & Balance:
- Adult ear conditions can arise from Congenital infections/ Syndromes, Genetic, Microtia/ Atresia and
Central Auditory Processing Disorder (CAPD) causes as for children.
(Read More: Children Services). - Age-related hearing loss – Natural wear and tear with degeneration of the inner ear and middle ear function is common in adults over 50 years of age, warranting screening for hearing loss. It is accelerated by noise exposure, certain drugs, infections and genetics.(Read More: Age-related Hearing Loss/ Presbyacusis); (Read More: How Hearing Loss Looks Like); (Read More: 10 things someone with hearing loss wish others know); (Read More: 10 Things to Know About Hearing Loss); (Read More: Age-related Hearing Loss/ Presbyacusis)
- Noise-induced hearing loss – This is due to very high noise level exposure for just a few minutes, or chronic high noise exposure. Some patients are more at risk due to genetics or poor general health e.g. hypertension and diabetes.(Read More: Noise-induced Hearing Loss); (Read More: Teaching Kids to Value Their Hearing)
- Tinnitus (ringing ears) – This is a result of hearing loss and may also occur due to tumors, abnormal vessels, thyroid dysfunction and drugs.(Read More: Tinnitus); (Read More: The Sound of Silence)
- Lumps and sinuses around/ on the external ear – These may be simple sebaceous cysts, keloids, pseudocysts or congenital preauricular sinuses.
- Ear wax – Impacted ear wax can cause discomfort and hearing reduction.
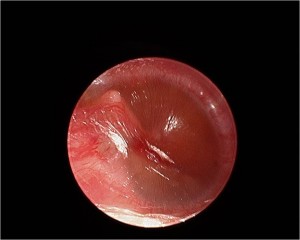
- Ear canal infection – This can arise from ear digging or trauma, swimming in dirty pools, skin pimple or abscess. Presents with foul smelling discharge and pain.(Read More: Ear Infections Adults)
- Otitis media – This can be acute, painful or accompanied with fever when associated with infections. Can be chronic with fluid in the middle ear, very often resulting from flights, diving, and associated with flu and cold. In rare cases, can be first presentation of a nasopharyngeal carcinoma (NPC). Very easily missed by even doctors, as changes in appearance of the ear drum may be subtle. May require hearing tests to confirm.
- Eustachian tube dysfunction – This can be due to anatomy, tone, nasal allergies or infections causing blocked ear sensations especially during descent of airplanes and at times of colds/ flu.
- Perforated ear drum – This can result from traumatic injury to the ear drum or chronic untreated middle ear and mastoid infections.
- Middle ear bones pathology – Malformed, dislocated, fractured, eroded, and fixed e.g. otosclerosis (fixed stapes). This can be congenital, traumatic, or due to chronic infection or tumor
- Cholesteatoma – A middle ear tumor that is not cancerous, but causes hearing destruction by eroding middle ear bones and bringing about toxin penetration to the inner ear. May erode into brain, face nerve and ear balance organs. Usually presents with recurring ear discharge.
- Malignant Otitis Externa – Bacterial infection of the ear canal and temporal bone causing deep pain and chronic ear discharge, often associated with diabetes and more common in the elderly.
- Mastoid infection – Chronic infection of the mastoid air cells and bony septations due to bacteria, fungus or unusual diseases like Tuberculosis.
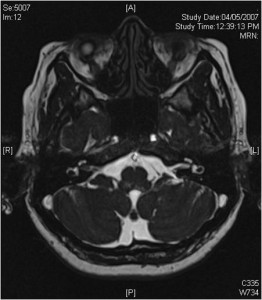
- Acoustic Neuroma – Tumor of the hearing nerve impairs hearing, and may cause facial nerve palsy, giddiness and increased intracranial pressure with growth.
- Microtia – Microtia auricle (malformed outer ear) and atresia ear canal (absent or narrowed ear canal) – A complex reconstruction challenge, with psychological, facial nerve, middle ear bones, hearing and cosmesis concerns. May have craniofacial disproportions or syndromes. Multiple combinations of management options need to be tailored to each patient’s anatomy and wishes.
- Giddiness – This is due to disorders in ear balance organs in about 30% of cases. This usually due to infections, Meniere’s Disease, Benign Paroxysmal Positional Vertigo (BPPV) and trauma. Other causes include drugs, brain, neurological, metabolic (e.g. sugar levels), heart and hormonal causes.(Read More: Dizziness and Vertigo); (Read More: When the Room Starts to Spin)
Significance:
- Hearing loss is often missed, and many do not seek seek ear balance treatment from an adult Ear Nose Throat specialist in Singapore for fear of stigmatization or deeming that it is not important.
- Many adults do not know they have hearing loss. It is often associated with ringing ears. Only 1 in 10 of adults requiring hearing aids uses them. There is a delay of diagnosis of 10 years on average. Beyond just increasing the risk of social isolation, depression and falls, hearing loss is now associated with memory/ cognitive impairment and dementia. In the National Health Survey 2010 study Dr Lim assisted with, 1 in 4 between 50-59 years of age; and 2 in 5 adults between 60-69 years old already have hearing loss. With each additional 10 years of life, the incidence increases dramatically.
- Many teenagers and young adults underestimate their noise exposure and the risk of noise-induced hearing loss. Many in professional jobs with noise exposure do not use hearing protection even if available. Have you had ringing ears after a cinema or clubbing event? That may indicate hearing loss that often starts at high frequencies. Listening to your music via headphones at maximum volume risks hearing loss in less than an hour.
Investigations offered:
The complete range of extensive hearing tests and services are available in-house in sound-proof and sound-treated rooms. Full-time audiologists in-house work closely with our Ear Nose Throat ENT doctor to interpret the tests together to tailor an optimal ear balance treatment plan the same day. This on-site real-time collaboration increases accuracy of diagnoses, safety during tests requiring sedation, and optimizes
outcomes.
- Otoscopy and light microscopy – Otoscopy offers clear views of the ear canal and ear drum. Light microscopy magnifies these images many times and with increased clarity for diagnosis.
- Adult hearing test – Pure tone hearing test, with and without hearing aids, speech discrimination, acoustic reflex threshold
- Eustachian tube dysfunction test – this can confirm if your inability to pop the ears or pressure pains especially on airplane descent or in lifts are due to a dysfunction of the cartilaginous-muscular tubes that connect your middle ears to the back of the nose
- Tympanometry – this test shows the middle ear pressure and volume, and is a reflection of the state of the ear drum and middle ear. It is often flat in patients with fluid or pus in the middle ear.
- Auditory Brainstem Response (ABR) and Auditory Steady State Response (ASSR) Tests – these electrophysiological tests examine the entire pathway of hearing, including that of the inner ear, hearing nerve, brainstem and cortical levels of the brain.
- Central auditory processing disorder CAPD tests – these are speech lists tests for adults with normal hearing but poor brain processing of sounds, usually requiring 2 sessions of 1-1.5 hours each under different conditions – e.g. in a noisy background or with competing sound information to both ears. Some with hearing loss can also benefit from CAPD tests in certain domains – this can improve outcomes of hearing aids use in selected patients.
- Radiology: CT scan temporal bone, MRI brain and Internal Acoustic Meatus are required to determine the anatomy of bony and soft tissue structures of the outer, middle and inner ear, cochlear, vestibular aqueduct, hearing and facial nerves and the brain. This also excludes infections and tumours.
- Genetic testing: There are over 200 types of genetic hearing loss. Contrary to common perception, 75% of newborns or young with hearing loss do not have parents or relatives with hearing loss. The only way to exclude genetic cause is to do an appropriate blood test guided by history. In Singapore, 40% of patients with unknown cause of hearing loss and other body systems normally have a Connexin 26 gene mutation. Knowing the genetic cause guides management over a lifetime, as there may be associated eye, kidney, heart or thyroid problems. It also suggests the progression and prognosis of hearing loss, besides helping families interested in determining the chances of hearing loss in future offspring.
- Tinnitus testing: Hearing tests include high frequencies testing. A Tinnitus Questionnaire and Tinnitus pitch matching.
Treatments Offered
NON-SURGICAL
- Non-surgical ear balance treatment such as topical ear drops, oral medications, and temporary cotton stents can help ear wax, and infectious, traumatic causes.
- Gentle ear cleaning and culture sensitivity of infection fluids, removal of wax and foreign bodies under light microscopic visualization and fine instrumentation.
- Hearing aids – a wide range of brands, sizes, types and degrees of sophistication, with customized choices for different ages and listening situations.(Read More: Hearing Aid Service); (Read More: 10 Ways Technology Improves Hearing Now); (Read More: 6 Things New Technology Hearing Aids Can Do)
- Customized ear and swim plugs
- FM systems for teachers, classrooms and halls to improve on HA performance. Personal and discrete Roger Pens microphone systems.
- Tinnitus treatment – Medications, education, psychological counselling, avoidance of stress factors and stimulating substances ( e.g. caffeine), tinnitus maskers, customized music therapy
- Central auditory processing disorder CAPD – Treatment has to be tailored and a multi-prong approach is needed: changing the learning or communication environment, recruiting higher-order skills to help compensate, and remediation of the auditory deficit itself (computer- assisted, one-on- one training with a therapist, home-based/ group programs
SURGICAL
- Non general anesthetic (GA) clinic procedures to help release pus or fluid from the middle ear in adults, or insertion of grommet tubes.
- Under GA (day surgery)- To release fluid or insert grommet tubes for glue ears
– To perform balloon eustachian tuboplasty- To repair perforated ear drums- To reconstruct or replace with simple prostheses for malformed or eroded ear bones/ stapes as in otosclerosis - Under GA (1 night stay)- To remove ear tumors that could be malignant or benign e.g. cholesteatoma- To eliminate chronic or dangerous mastoid ear infections via tympanomastoidectomy- To insert various implants (bone anchored hearing aids, middle ear implants or cochlear implants) (Read More: Cochlear and Middle Ear Implants); (Read More: We Felt Helpless, Lost); (Read More: The Invisible Hearing Device); (Read More: Did I Hear You Say Ear Implant?)
- Under GA (few nights stay):- To perform microtia and atresia surgery- For hearing: possible reconstruction of ear canal (canalplasty) and malformed ossicles (ossiculoplasty), or bone anchored hearing aids/ bone anchored active implants, or middle ear implants- For outer ear auricle reconstruction: choices include a prosthetic ear, Medpore (artificial graft) or patient’s own rib graft in the first stage, followed by the second stage with split skin graft from the abdomen and superficial temporal artery evascularisation.






