Children ENT Specialist in Singapore
Children are not just mini-adults. Their anatomy, health reserve, disease presentation, development and psychosocial needs differ across the age groups of newborns, neonates, infants, toddlers, young and older children and those in their teenage years.

The investigations frequently need to be more comprehensive, with the full armamentarium available, to tailor for newborns to children across all ages, and with different temperaments and stages of development. Extra time at the visit is needed. The concerns of and support from their family and caregivers are equally important. Coordinating care across multidisciplinary medical, educational and developmental bodies is also critical for best outcomes. This is possible with support from Dr Lynne Lim, an established Child Ear Nose Throat ENT specialist in Singapore with a strong network of equally established multi-disciplinary specialist colleagues. Her ENT specialist centre staff are experienced in caring for children.
After completing general ENT specialization in 2001, Dr Lynne Lim sub-specialized in Paediatric ENT at the renowned Cincinnati Children Hospital & Medical Centre, America, from 2001-2004, under the mentorship of the giant of Paediatric ENT, Dr Robin Cotton. The CCHMC ENT is an American Otolaryngology Board accredited world leader in Paediatric care, with strong subgroups of paediatric airway/ pulmonary/ swallowing; hearing/ speech and communication; snoring and syndromes; sinus and allergy; head and neck tumor management, research and education. It has a proud tradition of training many of the alumni leaders in paediatric ENT worldwide.

Ear / Balance / Tinnitus
Conditions managed Newborn – hearing loss – Can occur due to congenital infections (e.g. Rubella, CytoMegaloVirus, Toxoplasmosis, Herpes, Syphilis) or genetic causes with or without syndromes. Associated with

Ear / Nose / Throat Allergy
An allergy happens when our body’s immune system produces an exaggerated response to a normally harmless substance (allergen). An overwhelming response with antibodies results in
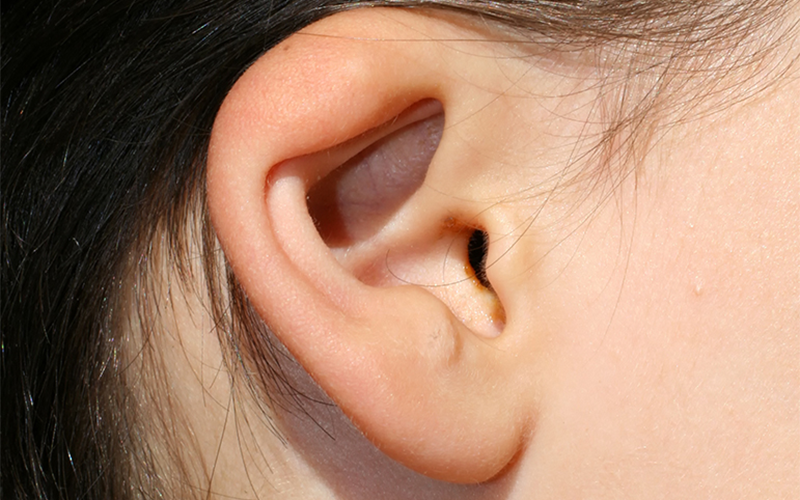
Ear Well for Malformed / Deformed Ears
Some babies may be born with outer ears that are malformed (smaller or constricted). Others may be born with ears that are deformed (differently shaped,
Head / Neck
A. Head and neck lumps Causes:The most common lumps are neck lymph nodes swelling from infections and congenital thyroglossal and branchial cysts. Other lumps are

Hearing Loss
Why do so many children get ear infections? And at what point do you consult a doctor or specialist? In this second of our specialist

Hearing Test
New-borns and children of any age can have a hearing test, and our oldest patient is a spunky 104 year old. Our hearing tests are

Nose / Sinus / Allergy
Epistaxis CausesNasal causes are usually picking of the nose, especially with allergic rhinitis. It can be due to foreign body, polyp, tumor, nose bone deviation

Snoring / Sleep Apnea
For children, instead of snoring, many have open mouth breathing as their nose passages are tiny. The child is restless, tossing and turning in sleep

Throat / Mouth
Tonsil and adenoid enlargement or infection Causes:Tonsils and adenoid enlargements in children may have intrinsic, unknown or infective origins. Importance:Adenoid and tonsil enlargement may result

Tonsils and Adenoids
8 Things to Know The tonsils and adenoids are lymphoid tissue that trap bacteria and viruses in the sides of our throat and the back






